.JPG)
| Our Guest Speaker Dr. Tony McMullen with President James Hamilton |
Dr. Tony was introduced by his brother Tim, a member of our club. Tim told us that his brother is married to Veronica and has two children and has a resume that reads:
•Born and Educated in Wagga, Married with 2 children
•Medical Education at Royal College of Surgeons in Ireland 1984
•Member of the RACGP & Australasian College of Tropical Medicine
•Master of Public Health & Tropical Medicine James Cook University 2001
•Work:
–Royal Flying Doctor Service & Aboriginal Medical Services in WA, NT & Qld
–Ireland, France, Botswana, Vietnam
–Indonesia since 1997, mainly as health advisor with large resource construction projects
•Newmont (Copper/Gold, USD2Billion), BP (LNG, USD5Billion)
–Medical Director BP South-East Asia
–Founded Persada Children’s Health in 2005
–Returned to live and work as GP in Sydney 2009
Tony came to talk about his work in West Papua where he founded Persada Children's Health also known as ASP which is an acronym for the Papuan translation of Persada Children's Health.
West Papua has been a passion for Tony since 1997 when he came across a boy named Ronaldo who had a congenital heart defect. Tony was working for a large company at the time and was able to raise funds to send Ronaldo to Singapore for life saving and life changing surgery.
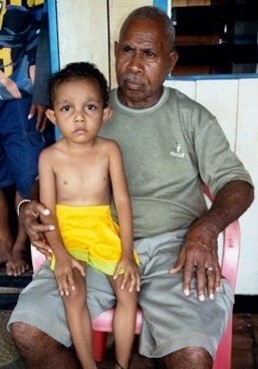  |
| Ronaldo on his grandfather's knee, a sick little boy and right Ronaldo as a healthy young teenager |
After Ronaldo's surgery, there was an amount of money left over, so Tony decided to start a foundation and since then numerous children have been sent to other countries for life saving surgery.
The foundation is situated in Sorong, the largest city in West Papua with a population of 220,000. It targets Malaria reduction and the treatment of Rotavirus, a diarrhea causing virus responsible for the deaths of many young children and infants. ASP deals with Malaria by treating the patients as vectors of the disease and effecting a cure in the individual patients. The reduction in Malaria cases has been dramatic.
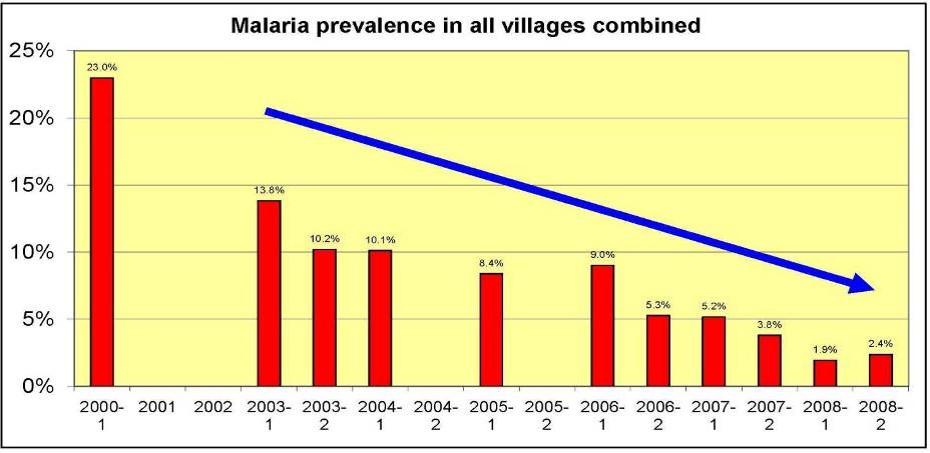 |
Malaria prevalence surveys in BP Tangguh villages Teluk Bintuni, Papua, from 2003-2008 |
These are the health statistics that Dr Tony gave us regarding health in West Papua.
•Children:
–Deaths of children in the first year of life almost 2 times the Indonesian average
–The Under-5 death rate is more than twice the national average
–4 out of 10 children of children are stunted
–One quarter are under-weight
•Health Equity:
–Just over 1/3 children receive their complete basic immunization
–Only 4/10 health centres are able to provide sufficient numbers of doctors
–Only 1/8 health centres are able to provide sufficient numbers of midwives
–Only 4/10 of health centres are able to provide sufficient numbers of nurses
•Water, Sanitation & Hygiene:
–4/10 people don’t have access to safe drinking water
–More than ½ don’t have access to improved sanitation
•Infectious Disease:
–1/10 people still suffer from Malaria
–Just over half of the population are immunized against Polio (*****)
–3/10 people do not receive immunization against TB
Tony feels that the best approach to tackling these issues is through a business model rather than a charity model.
The aim is obviously to reduce poverty, access to clean water and sanitation and provide the very basics for a decent safe life.
What can we as Rotarians do to help?
"A strategic, well-managed collaboration between Rotary Against Malaria, ASP, local government & the private sector could make a very significant impact on Malaria transmission in West Papua"
1.Collaboration of Rotary Against Malaria, ASP, local government, private sector
2.Improve surveillance systems
–Identify ‘hot spots’ of Malaria in Papua Barat
–Prevalence surveys, develop strategic plan, pilot program
–Training of health staff on detection and reporting of new cases
3.Train EDAT Malaria Workers
–To ensure early detection and treatment as the most effective method of reducing malaria
–Train Microscopists
4.Employ a ‘gold standard’ Microscopist for cross-checking
5.Mid-term goal: Demonstrate success of pilot program, build local government capacity, influence government policy & eventual ‘ownership’ of the program.
What would this cost?
1.Improve surveillance systems
•Cost of expert to train local health workers and Microscopists (AUD4,000)
2.Employ a local ‘gold standard’ Microscopist for a year (AUD10,000 pa)
3.Adopt a village
•Increase coverage with LLINs (?)
•Funding: Approximately AUD15,000 for first year
Could this be an opportunity for another Global Grant?
 |
| Perhaps we could help to put more smiles on the faces of our near neighbours. |